Testicular Self-Examination (TSE) involves a man examining his own testicles and scrotum for possible incongruences, lumps, or swelling in order to detect possible sexual disorders or dysfunctions.

As a rule, the general advice is to do a TSE on a monthly basis. Although recommendations vary, physicians typically suggest the use of monthly TSE for men between the ages of 15 to 55.
There are several reasons to do a TSE. The first, most common one is to detect testicular cancer at an early, potentially treatable stage. Testicular cancer usually presents itself with a painless testicular swelling or lump, or any change in shape, size, or texture of the testicles.
Other reasons to do a TSE may be to detect indirect inguinal hernias, varicocele, and infections that may affect the testicles.
How to Do a TSE
There are many different instructions around of how exactly to do a TSE (there’s no general medical standard), and we recommend that you just look for it on the Internet to compare different descriptions and find the best way for you.
In any case, here below we briefly give you the idea of what to look for and what to do in a TSE.

Now, a TSE is typically done at home while standing in front of a mirror (to also see the testicles from different angles) and after a warm bath or shower or after using warm herbal compresses. Warmth may help to relax the skin of the scrotum and usually makes the structures within the scrotum easier to feel.
Perhaps needless to say is that you actually first need to become (be) familiar with the way your scrotum and testicles are shaped, feel and look like in their healthy condition. This is your baseline, as it were.
Okay, here we go. Now, first you would visually examine the scrotum and testicles for any skin or shape changes or visible swelling. You should look at them directly, but also in the mirror.
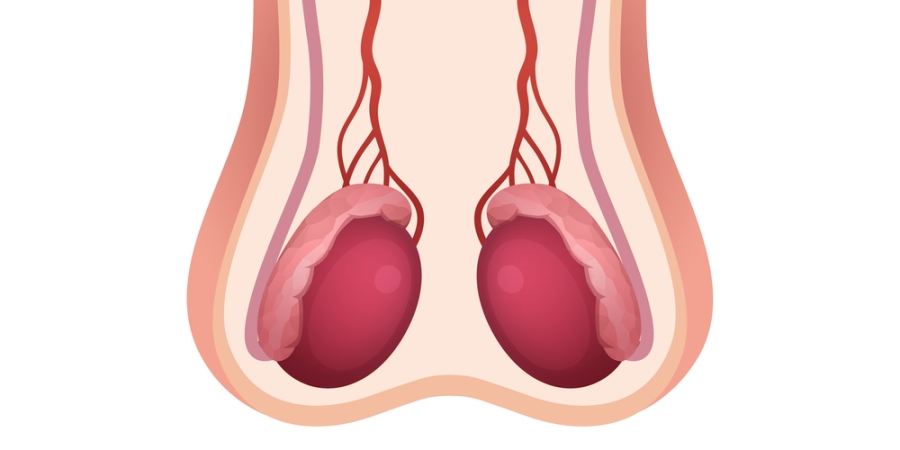
Afterwards, each testicle can be gently rolled between the thumb and fingers to feel for possible findings. Normal findings are that the testicles feel round, smooth, and homogenous in texture, and are mobile within the scrotum. In addition, there should be no pain or discomfort when the testicles and scrotum are handled gently. Mind that it’s normal for one testicle to be larger and hang lower in the scrotum than the other.
It’s also important to understand where the soft, rope-like epididymis is located (the little tightly curled tube at the back of each testicle that joins the vas deferens tube) and how it feels because it has a rather specific structure that could easily be confused as an abnormal finding.

Observations that may be abnormal and should be discussed with a physician or urologist are pain, discomfort or tenderness to the touch, hard or firm lumps, swellings or fluid buildup, changes in testicular size or the relative size of both testicles.
Mind that some signs and symptoms associated with testicular cancer may belong to other types of disorders of the male urinary tract and reproductive organs (such as urinary tract infections, cysts, epididymitis, varicocele, spermatocele, or sexually transmitted infections), so it’s important not to panic or get anxious before having consulted a healthcare professional.
If the abnormality is due to testicular torsion (twisted testicle) you will need immediate medical attention. Nevertheless, it’s not so hard to identify when this is the case because it’s a very painful condition and you will feel that at least one testicle is totally out of place.